We’ve all grown up hearing about various illnesses and infectious diseases…some small, many major.
But, as West Indians, especially Trinbagonians, we are accustomed to resorting to all sorts of anecdotes about what “granny” used “back in the day” to cure a problem, or of “bush” medicines that could remedy it all.
Common colds…we can beat that! A little fever…we have the bush for that too!
But, in the 21st century, with numerous illnesses, infectious diseases, epidemics and now a pandemic, beating even the smallest of illness seem to be but a major fight.
So where do we stand?
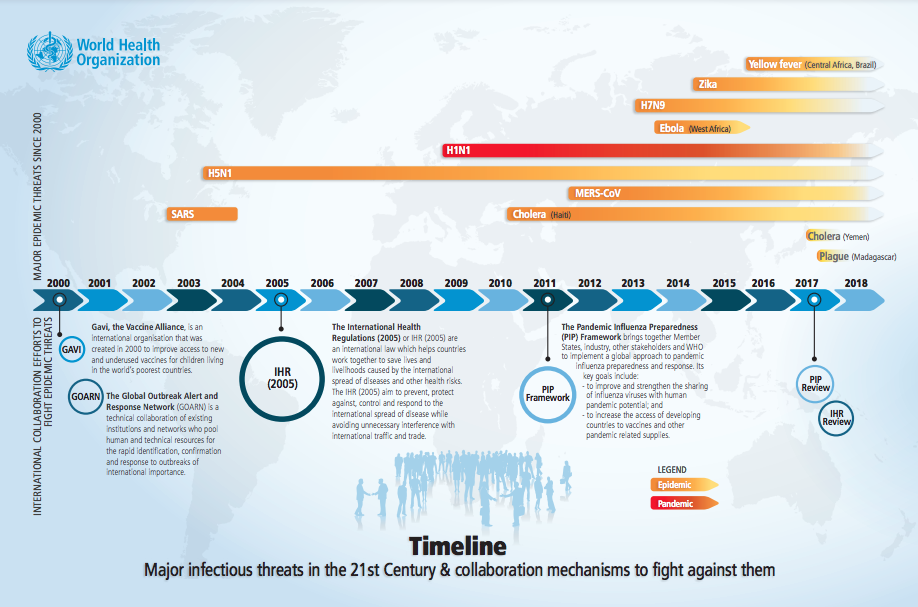
Already in these first two decades of the 21st century, the world has been sharply reminded time after time of the degree to which people in all countries and on all continents remain chronically vulnerable to infectious diseases, known and unknown.
Looking at a World Health Organisation study on Managing Epidemics, we at izzo realized that the Coronovirus is just the beginning and we have to learn to start LIVING with epidemics and taking the necessary precautions.
In this series we will look at diseases in the past and what we can expect going forward.
WHO reports that in the 1970s, and for years afterwards, remarkable progress, including the development of new vaccines, antibiotics and other treatments and technologies, led to a proclamation of a victory of mankind over microbes. Many experts thought it was “the time to close the book on the problem of infectious diseases” (Jesse Steinfeld, MD, US Surgeon General, 1969).
But… that was the experts “jumping the gun” as we would say as this lay the roots of a dangerous complacency.

The microbes they thought vaccines and antibiotics would eliminate didn’t go away. They just went out of sight.
Instead, the focus turned to chronic, non-communicable diseases, which came to receive much more attention. But nature was by no means in retreat. In fact, it seemed to return and took many health institutions and decision makers by surprise.
WHO says that since 1970, more than 1,500 new pathogens were discovered, of which 70% proved to be of animal origin: a connection that deserves renewed scrutiny.
Not all of them have had a public health impact but some of them have become famous. They included the Ebola virus, in 1976, and the human immunodeficiency virus (HIV), in 1983.
Pause for a moment and reflect that HIV, a relatively new disease in human history, has infected about 70 million people in just 35 years, and killed an estimated 35 million people in the same period. Consider also that in the last 40 years, Ebola has surfaced in almost 25 separate and deadly outbreaks, often after long spells in which it has apparently lain dormant.
These diseases have been selected because they represent potential international threats for which immediate responses are critical. Nearly all of them are subject to WHO’s International Health Regulations (2005) monitoring, and are part of the Global Health Security Agenda.

Will history repeat itself?
The answer must be: Yes, it will. A new HIV, a new Ebola, a new plague, a new influenza pandemic are not mere probabilities. Whether transmitted by mosquitoes, other insects, contact with animals or person-to-person, the only major uncertainty is when they, or something equally lethal, will arrive. The obvious follow-up question is: So what are we doing about it?
In order to try to see the road ahead more clearly, we need frequently to look over our shoulders – all the more so, because these early years of the 21st century have already been deeply scarred by so many major epidemics. Take plague, one of the most ancient scourges. A thing of the past? By no means. A major outbreak in Madagascar in 2017 led to a total of at least 2,417 confirmed, probable and suspected cases, including 209 deaths. Most cases were of the more fatal pneumonic type which is also transmissible from person to person, but there were also several hundred cases of bubonic plague.
Nine countries and territories with trade and travel links to Madagascar were put on plague preparedness alert.
The lesson here is that, over time, diseases very rarely disappear. And there always seems to be room for new ones. SARS – Severe acute respiratory syndrome – was unheard of before 2003. But it affected more than 8,000 people, killing about one in ten of them, causing fear and panic across the world, and inflicting enormous economic damage, especially in Asian countries.
In 2009, a novel influenza virus, H1N1, started to spread, creating the first influenza pandemic of the 21st century. But – and this is a reason for cautious hope – it was not as severe as expected thanks to recent preparedness efforts.
In 2012-2013, a new virus surfaced in the Middle East, causing an epidemic of what became MERS – Middle East respiratory syndrome – that spreads fatally into many countries beyond that region.
The Ebola epidemic in West Africa (Guinea, Liberia, and Sierra Leone) in 2014 was unlike the previous 24 localized outbreaks observed since 1976. Instead of being restricted geographically, this one seriously affected three African countries and spread to six other countries in three continents, and sparked alarm worldwide.
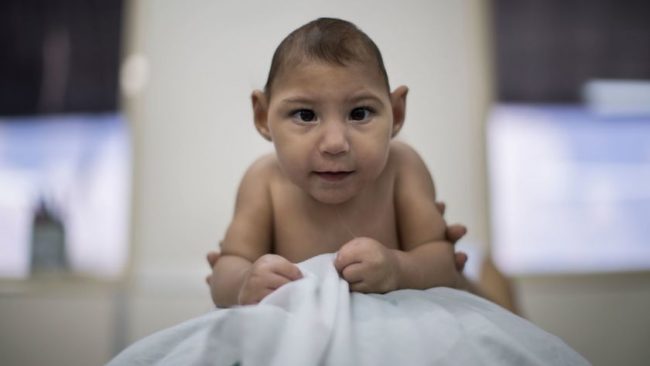
Baby with “Zika”
In 2015, the Zika virus, transmitted by the Aedes Aegypti mosquito, triggered a wave of microcephaly in Brazil. This disease causes dreadful damage in the brains of unborn babies. Almost 70 countries, one after another, then experienced their own Zika epidemic.
There are probably many more to come, because most of the global intertropical zone has a high density of Aedes Aegypti that transports the disease. And so a clear pattern continues to take shape. Old diseases – Cholera, Plague, Yellow fever among them – often return, and new ones invariably arrive to join them. About 40 outbreaks of cholera alone are reported to WHO every year
Faster and further with a greater impact. This pattern has another, deeply troubling aspect. The epidemics in the 21st century are spreading faster and further than ever.
We will tackle that in our next article…


COMMENTS